Cyanotoxins & Human Health
There are many species of cyanobacteria that produce toxins, often called cyanotoxins. Not all species are toxic, and the presence of a bloom does not always indicate that toxins are present. Additionally, there can be multiple strains of the same species, and while one strain may produce toxins another may not. Further, some species only produce toxins under certain environmental conditions. The only way to accurately know if toxins are present is to collect samples and preform laboratory analyses.
Cyanotoxins can be grouped into 4 categories (toxins in bold are most common):
- Hepatotoxins: toxins that disrupt liver functioning
- Microcystins
- Nodularins
- Cylindrospermopsins
- Neurotoxins: toxins that affect the central nervous system
- Anatoxins
- Saxitoxins
- BMAA
- Dermatotoxins: toxins that produce rashes and reactions on skin
- Endotoxins: cause gastrointestinal irritation
Signs and symptoms vary based on route of exposure and the type of cyanotoxin present, but include gastrointestinal effects such as nausea and vomiting, sore throat, headache, skin rash, swollen lips and muscle weakness. Find a more detailed evaluation of potential health concerns of cyanobacteria by the state of MA here.
Routes of exposure
Human health risk from exposure to cyanotoxins during recreational water use arises via three routes of exposure:
- Direct contact of exposed parts of the body, including sensitive areas such as the ears, eyes, mouth and throat, and the areas covered by a bathing suit.
- Exposure is heightened if cuts or open wounds are present.
- Accidental swallowing of water containing cyanobacteria cells.
- Uptake of water containing cells by aspiration (inhalation)
- EPA concluded that inhalation exposure is negligible compared to incidental ingestion while recreating, details here.
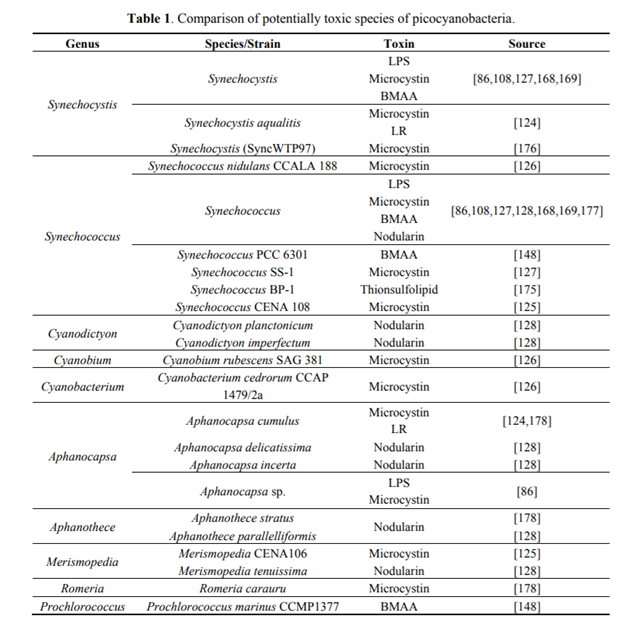
BMAA-ALS Hypothesis
A link has been suggested between the amino acid β-N-methylamino-L-alanine (BMAA) and neurological degradation, and some older studies found a correlation between BMAA consumption via food and to the neurological diseases ALS and Parkinson’s. In particular, a correlation was found between BMAA and an ALS hotspot in Guam. A review of these studies can be found here.
A few studies suggest a correlation between ALS and BMAA, but causation has not been proven, and more recent science suggests that this connection is not real.
While the science is still emerging, the evidence linking cyanobacteria to neurological diseases is weak and BMAA is not monitored as a toxin by the EPA, WHO, or any state in the U.S. Here are the reasons the evidence is considered weak:
- The high incidence of ALS in Guam was linked to consumption of the poisonous Cycad plant, which harbors cyanobacteria in its roots. This route of exposure led to very high levels of BMAA intake, as well as other environmental toxins produced by the plant.
- The initial studies which found BMAA in the brains of Guam ALS patients used analytical techniques to measure BMAA that are now obsolete and less accurate than today’s methods.
- Consumption of cycad trees was widespread in indigenous Guam culture, yet the ALS hotspots were limited to certain areas. If ALS was linked to consumption of the cycad plant, then ALS would have been more widespread.
- Patchiness of ALS incidence suggests there may have been another factor leading to ALS, such as the levels of minerals and metals in the soil and/or water.
- The type of ALS observed in Guam has a different pathology compared to classic ALS observed elsewhere and is likely a unique disease and not relevant to ALS in other localities.
- Toxicity studies linking BMAA to neurodegeneration in rodents and primates used very high BMAA concentrations (>100 uM) that are not physiologically relevant.
- Dosage that elicited neurotoxicity is way higher than environmental exposure to cyanobacteria. It is not relevant to dosage humans would be exposed to, even if they drank water with cyanobacteria.
- Dosage given to animals in study was many magnitudes higher than what is environmentally relevant.
- Exposure method was not relevant, being injected or force-fed high levels of BMAA is not comparable to exposure via consumption, inhalation or exposure via cuts in skin.
- Dosage that elicited neurotoxicity is way higher than environmental exposure to cyanobacteria. It is not relevant to dosage humans would be exposed to, even if they drank water with cyanobacteria.
- Cyanobacteria are ubiquitous and blooms have been occurring for centuries (written accounts by Romans and Egyptians of blooms). If there was indeed a link between cyanobacteria and ALS, the disease would be much more widespread.
- Cyanobacteria are very likely found in the drinking water of developing countries. This direct exposure would lead to increased incidence of disease, if there was a causal link between neurodegenerative diseases and cyanobacteria.

